Table of Contents
What Happens During a CPAP Follow-up
Congratulations, you have successfully started your CPAP (Continuous Positive Airway Pressure) sleep therapy to alleviate your sleep apnea and all the associated health complications it causes. But if you are like many new CPAP machine users, your first nights wearing your mask may feel clumsy, uncomfortable, or even claustrophobic. These forms of issues result in as many as 50% of all CPAP patients having difficulty sticking with their therapy program.
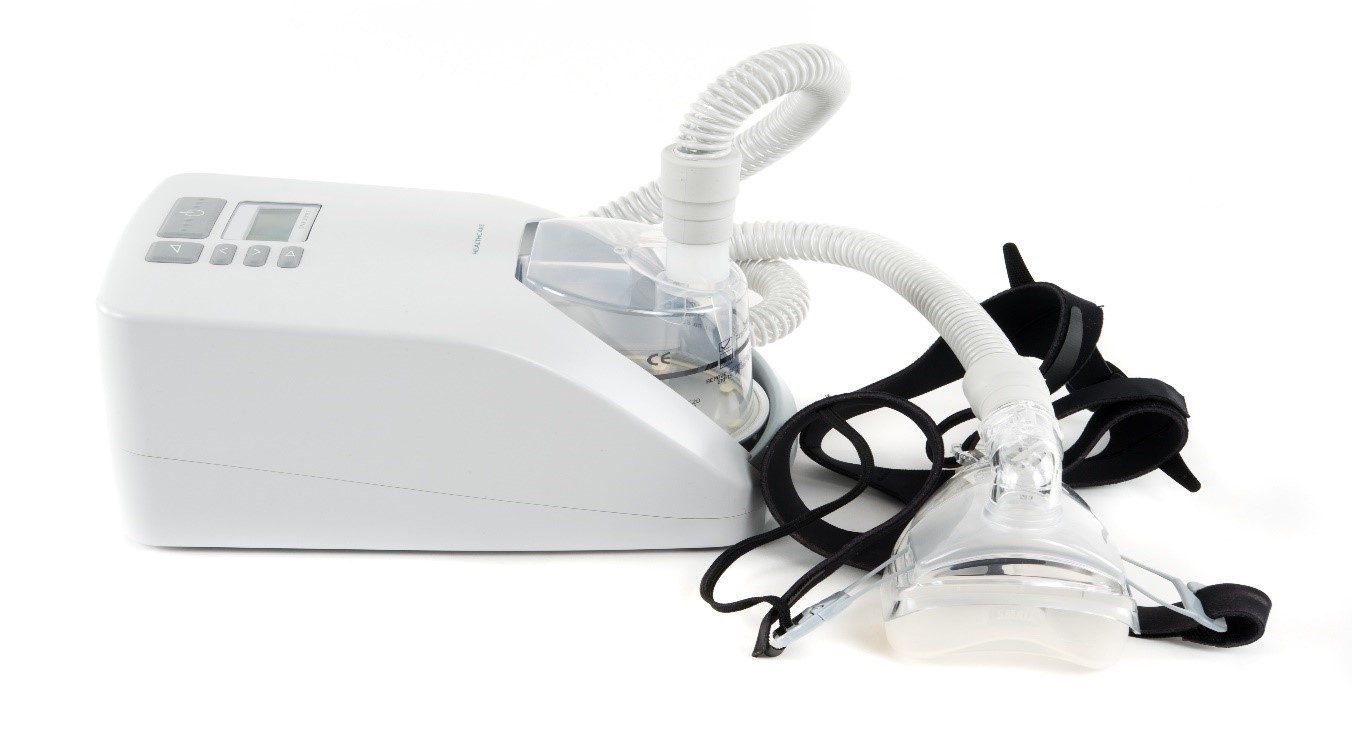
This is why CPAP follow-ups are a crucial part of your treatment program. Your doctor and sleep medicine professional are well-acquainted with all of the issues reported by CPAP users and are a helpful resource in helping you to succeed. Their solutions may be as simple as learning how to fit a CPAP mask correctly, adding a humidifier/heater unit, or implementing an “acclimatization strategy” to ease you into its utilization. All these are made possible through CPAP fitting appointment.
Phase 1: Early Follow-ups
The most crucial follow-up comes in the form of a phone call within 24-48 hours of your first use of your new CPAP machine. Be prepared to tell your physician everything, particularly if you are having any trouble. You might be asked about the following:
- Mask comfort problems. Is your mask comfortable? Are you feeling any roughness? Are you having trouble keeping it on while asleep?
- Equipment problems. Is the air pressure too weak or too strong? Do you wake up with dry throat, mouth, or nostrils? Is the length of hosing interfering with your sleep? Is the noise of the CPAP disturbing?
- Medical issues. Are you feeling more rested? Has your daytime sleepiness enhanced? Are you still snuffling or suffering sleep apnea, where you stop breathing?
- Miscellaneous issues. Does your bed partner have any worries or questions?
Your physician will use your answers to suggest adjustments that can alleviate these issues.
One of the most popular and most effective fixes is to loosen your mask’s straps. An over-tight mask is actually more likely to create loose seals, which decrease your CPAP’s efficiency.
At the 1-week follow-up, you can attempt switching the size, style, or type of mask you are using, adding or removing padding, or even changing to another model of CPAP/Bipap machine. In addition, your doctor can provide other non-equipment recommendations on subjects like:
- Good sleep hygiene behaviors
- Attendance at help groups
- Desensitization methods of wearing a mask
- Guidelines for falling asleep and extending sleep
- Suggestions on how family/bed partners may help
Remember, do not get discouraged! An adjustment period is perfectly reasonable, and it will be different for every person. For some, getting used to sleeping with a CPAP will take some days; others will need multiple adjustments, fittings, adaptations, etc. that may take several months.
Phase 2: Ongoing Followups
At the 1-week, 2-week, 6-week, and 6-month marks, your sleep medicine professional may ask you to bring in your CPAP, or its removable memory chip. This automatically records usage and other information that may be used in analyzing the effectiveness of your CPAP therapy.
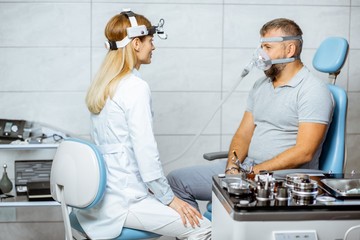
You may expect to be asked similar questions as in your early follow-ups. At these times, you may also discuss issues like:
- Appropriate cleaning of PAP unit and accessories
- Checking for the fitting of the mask
- Equipment and parts replacement recommendations
- Weight gain, weight loss, alcohol consumption while using your CPAP
Phase 3: Yearly Follow-up
If all goes well, this annual follow-up can simply be a fast formality. Your physician will check for:
- Any physical changes that may necessitate a new mask
- Maintenance check on your CPAP machine, ensuring it is functioning properly
- Information about new equipment, as well as masks and CPAP machines.



 Shop
Shop