Table of Contents
Central Sleep Apnea Causes
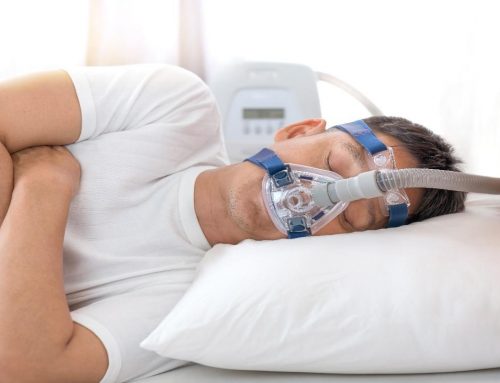
Central sleep apnea is a disorder in which your breathing continuously stops and starts during sleep. Central sleep apnea happens because your brain doesn’t send required signals to the muscles that control your breathing. This condition is distinct from obstructive sleep apnea, in which you can’t usually breathe because of upper airway obstruction. Central sleep apnea is less prevalent than obstructive sleep apnea.
It may occur due to other conditions, such as heart failure and stroke. Sleeping at a high altitude also may lead to central sleep apnea. Treatments for central sleep apnea may include treating existing conditions, using a device to aid breathing, or using supplemental oxygen.
Symptoms
 Common signs and symptoms of central sleep apnea include:
Common signs and symptoms of central sleep apnea include:
- Observed episodes of halted breathing or unusual breathing patterns during sleep
- Abrupt awakenings coupled with shortness of breath
- Shortness of breath that’s easens when sitting up
- Difficulty staying asleep (insomnia)
- Excess daytime sleepiness (hypersomnia)
- Chest pain at night
- Difficulty concentrating
- Mood swings
- Morning headaches
- Snoring
- Lower tolerance for exercise
Although snoring shows some degree of airflow obstruction, snoring also may be experienced in the presence of central sleep apnea. Moreover, snoring may not be as prominent with central sleep apnea as it is with obstructive sleep apnea.
When to see a doctor
See a medical professional if you experience, or if your partner notes any signs or symptoms of central sleep apnea, especially the following:
- Shortness of breath that disrupts your sleep
- Intermittent pauses in your breathing during sleep
- Difficulty staying asleep
- Extreme daytime drowsiness, which often leads to falling asleep while you’re working, watching television or even driving
Causes of Central Sleep Apnea
 The cause depends on the type of central sleep apnea you have. They include:
The cause depends on the type of central sleep apnea you have. They include:
- Cheyne-Stokes breathing.
This kind of central sleep apnea is most often associated with congestive heart failure or stroke. Cheyne-Stokes breathing is noticed by a gradual increase and then a reduction in breathing effort and airflow. During the weakest breathing effort, an absolute lack of airflow (central sleep apnea) can occur.
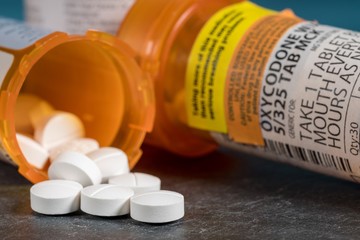
- Drug-induced apnea.
Taking certain medications such as opioids such as morphine (Ms. Contin, Kadian, others), oxycodone (Roxicodone, Oxycontin, others), or codeine may lead to your breathing to become irregular, to increase and decrease in a steady pattern, or to temporarily stop completely.
- High-altitude periodic breathing.
Cheyne-Stoke breathing pattern may happen if you’re exposed to a very high altitude. The change in oxygen at this altitude causes alternating rapid breathing (hyperventilation) and under breathing.




 Shop
Shop