Table of Contents
Do I Really Need CPAP Treatment?
Sleep apnea is a common condition that disrupts breathing during sleep, often leading to pauses followed by gasping or choking. Those aware of these events may say they wake throughout night feeling like they simply can’t breathe, but many are only made aware of such breathing disruptions because their partner notices them.
Instances of stopped breathing while asleep that last 10 seconds or more are called apnea events. If episodes of that duration only involve partially blocked breathing during sleep, they are called hypopnea events.
Having five or more such events a night is considered abnormal.
Symptoms of Trouble Breathing

During an apnea event, your breathing stops while you are asleep. You are unaware of it at that point.
To restore your breathing, you come out of sleep and may choke, gasp, and breathe loudly and fast. You may sometimes fully awaken and be aware of this happening, feeling like are being smothered and need to restore your breathing. But it’s possible that you may not wake up completely, or that you may go back to sleep and not remember the apnea event in the morning.
Partially blocked breathing in a hypopnea event might result in snoring. While snoring can happen without hypopnea, it is one of the most common symptoms of sleep apnea.
If these instances of stopped breathing happen frequently during the night, you are likely to feel like you slept terribly.
Day-time symptoms of trouble breathing at night include:
- Dry mouth
- Sore throat
- Morning headache (due to the retention of carbon dioxide during sleep)
- Excessive sleepiness (e.g., you may fall asleep during meetings or even while driving)
- Poor concentration
- Memory dysfunction
- Mood problems
Children with sleep apnea may show signs such as:
- Mouth breathing
- Bedwetting
- Sleepwalking
- Restlessness
- Sweating during sleep
They may also have growth problems and attention deficit hyperactivity disorder (ADHD).
Causes
There are two main types of sleep apnea that can result in breathing stoppages while you sleep. These are obstructive sleep apnea and central sleep apnea.
Obstructive Sleep Apnea (OSA)
During sleep, your upper airway (the tissues surrounding the throat, including the soft palate and base of tongue) relax and narrow, but this should not be enough to block your airway.
Obstructive sleep apnea occurs when the upper airway partially or completely collapses and blocks the ability to breathe. An effort to breathe continues, but air is not moving through the nose, mouth, and throat to the lungs.
This leads to a drop in the blood oxygen levels and a sudden awakening is needed to activate the muscles in the upper airway to restore normal breathing. Snoring, in fact, is the result of the tissues relaxing so much that they vibrate during breathing.
Factors leading to obstructive apnea include structural causes that result in a smaller upper airway, such as enlarged tonsils, a soft palate that hangs low, or nasal obstruction.
Being overweight and having a large neck are also risk factors.
Central Sleep Apnea
Central sleep apnea is not caused by an airway blockage but by a failure of the respiratory control center of the brain.
Your brain must signal your muscles to breathe, and this function can be impaired in neurological disorders such as amyotrophic lateral sclerosis (ALS) and conditions such as heart failure.
Drugs such as opiates also suppress the respiratory center and can produce central sleep apnea while they are in your system.
Diagnosis
If you or your partner have noticed frequent episodes of stopped or troubled breathing during sleep, or you have symptoms that this may be occurring, discuss it with your healthcare provider.
Your doctor will take your medical history and a report of symptoms, as well as conduct a physical examination.
If sleep apnea is suspected, a referral to a board-certified sleep specialist will be made. They will then conduct a thorough assessment of your symptoms and, likely, a diagnostic sleep study.
Sleep Study
A sleep study will identify the episodes of stopped breathing during sleep. This may be done at home or at a sleep center.
During this test, electrodes are placed on your eyelids, scalp, and chin, and chest monitors record your breathing and heart rate. During sleep, the number of times you stop breathing (apnea events) and almost stop breathing (hypopnea events) are recorded. Other observations are made regarding movements as well.
The apnea-hypopnea index (AHI) is used to make sense of the results. The number of apnea events and hypopnea events is totaled to calculate an AHI score.
An AHI score of less than 5 is considered normal. A higher score indicates that you have sleep apnea.
Further evaluation will help determine the cause of your sleep apnea and guide what treatment is appropriate.
Treatment

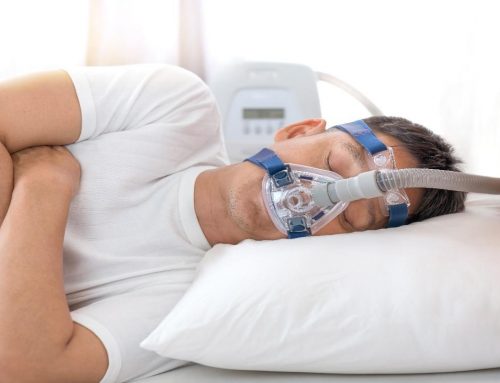
The most common and effective treatment option for sleep apnea (particularly moderate to severe) is continuous positive airway pressure (CPAP). Bilevel positive airway pressure (BiPAP) may also be considered. Both deliver a flow of air through a face mask while you sleep.
Other options, from weight loss to dental devices to surgery, may also be considered.



 Shop
Shop