Table of Contents
FDA CPAP Machine Reclassification
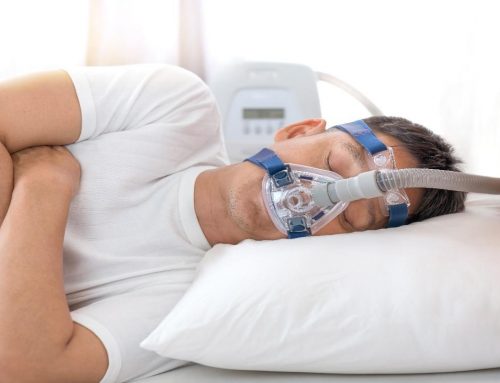
 The U.S. Food and Drug Administration (FDA) issued a final rule, “Classification of the Positive Airway Pressure Delivery System,” which was effected on Oct. 19, 2018, that re-categorized the positive airway pressure (PAP) delivery system, moving it from Class III into Class II. PAP delivery systems continue to be for prescription use only.
The U.S. Food and Drug Administration (FDA) issued a final rule, “Classification of the Positive Airway Pressure Delivery System,” which was effected on Oct. 19, 2018, that re-categorized the positive airway pressure (PAP) delivery system, moving it from Class III into Class II. PAP delivery systems continue to be for prescription use only.
The FDA generally groups medical devices depending on the risks associated with the equipment and by evaluating the amount of regulation that provides a reasonable assurance of the device’s safety and effectiveness. Class I devices normally pose the lowest risk to the patient, and Class III devices pose the highest risk. The major purpose of reclassification is to apply the correct level of regulatory controls for a device type based on the most current information concerning its safety and effectiveness.
All machines, including PAP delivery systems, that were not in commercial distribution before May 28, 1976, are automatically classified as and remain within, Class III, and need premarket approval unless and until FDA takes action to classify or reclassify the device. The PAP re-categorization came after the FDA received a de novo classification request from FRESCA Medical for the CURVE PAP system. Nevertheless, reclassification is applied to a particular device type and not an individual device. The FDA determined that the PAP delivery system can be grouped into Class II with the establishment of special controls, which will offer reasonable assurance of the safety and effectiveness of the device.
The FDA believes that placing the PAP device into a lower device class will improve patients’ access to beneficial innovation, partly by lowering regulatory burdens. The exceptional controls stipulated by the FDA for reclassifying the PAP delivery system to Class II are:
1. The patient-contacting components of the machine must be demonstrated to be biocompatible.
2. Non-clinical performance testing must prove that the device performs as intended under anticipated conditions of use, including the following:
- Waveform testing must simulate breathing conditions and assess pressure and airflow response over a range and combination of high and low breath rates and tidal volumes.
- Use life testing must prove adequate device performance over the labeled use life of the device.
- Device integrity testing must demonstrate that the machine can withstand typical forces expected during use.
- Carbon dioxide rebreathing testing must be done.
- System flow rate, maximum expiratory pressure, inhalation pressure, and intra-mask static pressure testing must be executed.
- Air bolus testing must demonstrate that the machine can withstand worst-case scenario air pressures.
- Maximum limited pressure testing of the flow generator in a single fault condition must be accomplished.
- Maximum output temperature testing of delivered gas, if humidified, must be executed.
 3. Performance data must authenticate reprocessing commands for any reusable components of the device.
3. Performance data must authenticate reprocessing commands for any reusable components of the device.
4. Performance data must demonstrate the electrical, thermal, and mechanical safety and the electromagnetic compatibility of the machine.
5. Software verification, validation, and hazard analysis must be done.
6. Labeling must comprise the following:
- Therapy pressure range;
- Use life and replacement schedule for all elements;
- Cleaning guidelines; and
- Instructions for assembly and connection of machine components.
According to the FDA rule, a PAP delivery system “is a prescription noninvasive ventilator machine that delivers expiratory positive airway pressure for patients suffering from obstructive sleep apnea. The system also offers positive airway pressure during incipient apnea. The system may consist of a dedicated flow generator and a patient interface.


 Shop
Shop